 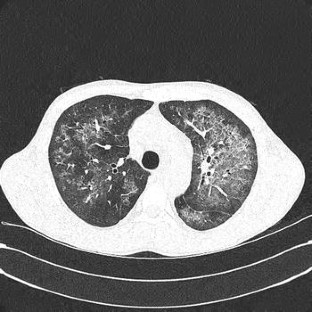
The complete blood count showed leukocytes 15,500/mm 3 (neutrophils 79.3%), hemoglobin 13.2 g/dL, platelets 229,000/mm 3, and erythrocyte sedimentation rate 5 mm/h. The patient underwent arterial blood examination while breathing 35% oxygen with a venturi mask and was confirmed to have a PaO 2/FiO 2 188 mmHg, PaO 2 65.8 mmHg, and oxygen saturation 94.1%. The muscular strength of both upper and lower limbs was confirmed as grade 5. On physical examination, crackle was heard from the lower lobes of both lungs. On admission, his vital signs were as follows: blood pressure 110/50 mmHg, pulse 103 beats/min, respiratory rate 18 breaths/min, body temperature 38.6✬, with clear consciousness. The patient was transferred to our hospital in Seoul with suspicion of rheumatic disease. Serologic tests for antinuclear antibodies were positive. He took oral levofloxacin but the symptoms did not improve furthermore, he continued to suffer from dyspnea. A week after the trip, he began to suffer from fever and chills and was diagnosed with pneumonia in another hospital. He lives in Los Angeles and a month before had travelled to Las Vegas for about a week. At the time of admission, he had rash on both sides of the pelvis and groin. Although he usually had a nonspecific whole-body skin rash and wax-and-wane myalgia, this had not been assessed. He was a current smoker of 5 pack years with no underlying disease. Case Report A 46-year-old man was admitted to the emergency room with dyspnea that had worsened during the preceding 10 days. Here, we report such a case and review the literature. Using immunosuppressive treatments such as high-dose steroid, cyclophosphamide and intravenous (i.v.) immunoglobulin, we have successfully treated patients admitted to hospital with COP and respiratory failure caused by dermatomyositis. Severe COP with respiratory failure caused by dermatomyositis is very rare, and treatment remains difficult therefore, it is important to share experience of successful treatment of patients in clinical practice. Moreover, immunoglobulin injection has shown efficacy in patients with severe interstitial lung disease (ILD), even though its mechanisms of action in dermatomyositis and polymyositis is not clear. However, when the clinical course in more aggressive and immunosuppressive agents including steroid, azathioprine, mycophenolate, cyclophosphamide and methotrexate are not very effective, immunosuppressive agents such as rituximab and tacrolimus can be used. Cryptogenic organizing pneumonia (COP) is a common pattern of pulmonary complication known to respond well to steroid treatment. The disease can involve the whole body including the respiratory system. heliotrope erythema, Gottron’s sign, Gottron’s papules) accompanied by erythema and edema, proximal muscle weakness of limbs and nonsuppurative inflammation. Dermatomyositis is an incurable connective tissue disease that results from inflammatory and degenerative changes in muscle and skin, it has several prominent symptoms, including skin lesions (e.g. Keywords: cryptogenic organizing pneumonia dermatomyositis immunoglobulins lung diseases, interstitialĪutoimmune reactions in connective tissue diseases cause systemic and have a significant impact on the survival of patients with pulmonary manifestations.However, the respiratory failure did improve after treatment with intravenous immunoglobulin, which therefore can be considered a treatment option in cases where steroids and immunosuppressive agents are ineffective. He was diagnosed with dermatomyositis combined with cryptogenic organizing pneumonia (COP) with respiratory failure and underwent treatment with steroid and an immunosuppressive agent, but the COP was not improved. In the present case, a 46-year-old man was admitted to our hospital with dyspnea. In such cases, the prognosis is very poor despite treatment with high-dose steroid. Dermatomyositis is an incurable, uncommon form of connective tissue disease that occasionally causes diffuse pulmonary inflammation leading to acute severe respiratory failure. In connective tissue diseases, autoantibodies cause pulmonary interstitial inflammation and fibrosis, and patients require treatment with an immunosuppressive agent such as a steroid.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
